Imagine waking up with a racing heart, shaking hands, and a sudden, unexplained weight loss that makes you feel like your body is running a marathon while you're just sitting still. For many, these aren't just signs of stress or caffeine overkill-they are the hallmarks of Graves' Disease is an autoimmune disorder that causes the thyroid gland to overproduce hormones, leading to hyperthyroidism. It is the most common cause of an overactive thyroid, accounting for roughly 80% of these cases. While the symptoms can feel overwhelming, understanding how the disease works and the role of medications like PTU can help you regain control over your health.
What is Actually Happening in Your Body?
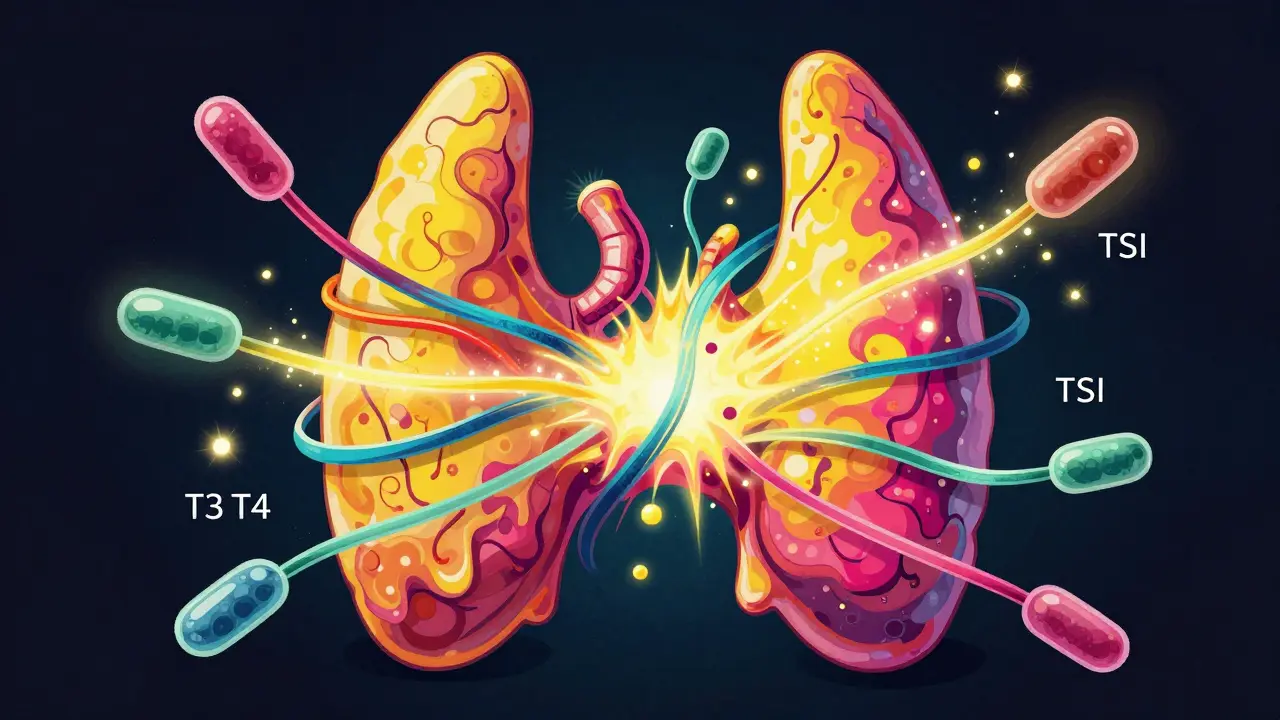
To understand Graves' disease, you first need to know about the Thyroid, a butterfly-shaped gland in your neck that acts as the body's metabolic thermostat. Normally, your brain sends a signal called thyroid-stimulating hormone (TSH) to tell the gland how much energy your body needs. In someone with Graves', the immune system glitches. Instead of fighting germs, it creates antibodies called Thyroid-Stimulating Immunoglobulin (TSI). These antibodies trick the thyroid into thinking it needs to work overtime, pumping out excessive amounts of thyroxine (T4) and triiodothyronine (T3).
This hormonal surge puts your body into overdrive. Because women are affected at a ratio of 7:1 compared to men-most often between the ages of 30 and 50-it's frequently misdiagnosed as severe anxiety or early menopause. If left untreated, this state of hyper-metabolism can lead to brittle bones and cardiovascular strain. In extreme cases, it can trigger a Thyroid Storm, a life-threatening crisis where heart rate and temperature spike dangerously, carrying a mortality rate of 20-30%.
Spotting the Signs: Beyond the Racing Heart
Hyperthyroidism is the most obvious part of the disease, but Graves' often comes with "extra" symptoms that other thyroid issues don't have. You might notice your eyes feeling gritty or looking more prominent. This is Graves' Ophthalmopathy, where inflammation causes the eyes to bulge (proptosis). In about 3-5% of cases, this can even threaten your vision by compressing the optic nerve.
Less common, but still possible, is a skin condition called dermopathy, which usually appears as thick, red skin on the shins. From a diagnostic standpoint, doctors look for a specific blood pattern: a very low TSH (often below 0.4 mIU/L) paired with high levels of free T4 and T3. To confirm it's actually Graves' and not another form of hyperthyroidism, they will test for TRAb (thyrotropin receptor antibody), which is accurate in over 95% of cases.
Decoding the Treatment: Why PTU?
When you're diagnosed, the goal is to bring your hormone levels back to a normal range (euthyroid status). Doctors typically use Antithyroid Drugs (ATDs) to block the production of hormones. The two heavy hitters here are methimazole and Propylthiouracil (PTU). While methimazole is the go-to for most adults because it's taken once a day and is generally safer for the liver, PTU has a very specific and critical role.
PTU is the preferred choice during the first trimester of pregnancy. This is because methimazole carries a higher risk of causing birth defects (teratogenic risk). Additionally, PTU works faster to lower hormone levels, making it essential for treating a thyroid storm. However, PTU isn't without risks. It carries a small but serious risk of severe liver damage (hepatotoxicity), which is why people on this medication need regular blood work.
| Treatment Option | Primary Action | Pros | Cons/Risks | Approx. Cost |
|---|---|---|---|---|
| ATDs (Methimazole/PTU) | Blocks hormone synthesis | Reversible, non-surgical | Liver toxicity (PTU), Relapse risk | $10-$50/mo |
| Radioactive Iodine (I-131) | Destroys thyroid cells | Fast, definitive | Permanent hypothyroidism | $300-$1,500 |
| Thyroidectomy | Surgical removal | Immediate resolution | Surgical risks, lifelong meds | $5,000-$15,000 |
Living with the Medication: What to Expect
Starting Propylthiouracil is a journey of monitoring. You won't just take the pill and forget it. Because of the risk of liver injury, about 68% of PTU users undergo monthly liver function tests (LFTs). You'll also need to keep an eye out for a rare but dangerous condition called agranulocytosis, where your white blood cell count drops. If you suddenly get a sore throat or a fever while on ATDs, you need to call your doctor immediately-these are the red flags that the medication is affecting your bone marrow.
The typical course of drug therapy lasts 12 to 18 months. During this time, your doctor will check your TSH every 4 to 6 weeks until you're stable. For some, this leads to remission-meaning the thyroid returns to normal and the meds can be stopped. However, the relapse rate is high, with 40-60% of people seeing symptoms return within a year after stopping the pills. This is why some patients eventually opt for the more permanent solutions of radioactive iodine or surgery.
Navigating the Emotional and Physical Toll
The physical symptoms are only half the story. A huge number of patients report severe anxiety, insomnia, and an irritability that can strain relationships. It's not just "in your head"; it's a direct result of your metabolism being overclocked. Weight loss is also common, with many losing 15-20 pounds before they even get a diagnosis. Because the symptoms mimic anxiety disorders so closely, many people spend months visiting therapists before they ever see an endocrinologist.
If you're struggling with eye issues, be aware that thyroid normalization doesn't always fix the eyes. About 40% of patients still have eye symptoms even after their hormone levels are perfect. For these cases, new treatments like teprotumumab have emerged, though they are incredibly expensive. The best approach is usually a team effort involving an endocrinologist and an ophthalmologist to manage the inflammation separately from the hormone levels.
Is PTU safer than methimazole?
Generally, no. Methimazole is the first-line treatment for most adults because it has a lower risk of severe liver toxicity and is easier to dose. However, PTU is significantly safer during the first trimester of pregnancy and is more effective for treating a life-threatening thyroid storm.
Can Graves' disease go away on its own?
It is very rare for Graves' to resolve without intervention. While some people enter remission after 12-18 months of antithyroid medication, the disease typically requires lifelong management or a definitive procedure like radioactive iodine or surgery to prevent relapse.
What should I do if I feel my symptoms returning?
If you notice palpitations, tremors, or sudden weight loss again, contact your endocrinologist immediately. They will likely order a TSH test and potentially check your TRAb levels to see if the disease has relapsed, which may require adjusting your medication dose.
Does smoking affect Graves' disease?
Yes, significantly. Smoking is strongly linked to the worsening of Graves' ophthalmopathy (eye bulging). In fact, smoking can double the risk and severity of eye complications, making smoking cessation a critical part of treatment for the eyes.
What is the "Thyroid Storm" and why is it dangerous?
A thyroid storm is an extreme exaggeration of hyperthyroidism. It's a medical emergency where the body is flooded with thyroid hormones, leading to extreme tachycardia, high fever, and confusion. It has a 20-30% mortality rate if not treated aggressively with drugs like PTU and beta-blockers.
Next Steps for Patients
If you've just been diagnosed, your first priority is establishing a baseline with your doctor. Make sure you have a clear schedule for your blood tests-especially if you are on PTU-to monitor your liver and white blood cell counts. Keep a daily log of your heart rate and temperature; if your resting heart rate consistently exceeds 100 bpm, it's time for a medication review.
For those planning a family, be proactive. Discuss the switch from methimazole to PTU with your doctor before you conceive, as the timing of this transition is critical for fetal safety. If you find that the emotional toll of anxiety and insomnia is too high, ask your provider about beta-blockers, which can manage the heart racing and tremors while the antithyroid drugs take a few weeks to kick in.
Quinton Bangerter
April 22, 2026 AT 11:09Classic Big Pharma playbook right here. They push these ATDs to keep you in a loop of 'monitoring' and monthly blood tests just to secure a recurring revenue stream. Why do we trust the TSH baseline when the entire diagnostic framework is designed to maintain patient dependency? It's all a systemic failure of the medical industrial complex to acknowledge root causes over symptom management.
Ms. Sara
April 23, 2026 AT 09:19It is so crucial to emphasize the mental health aspect here. Living with this kind of systemic imbalance is exhausting and often invisible to others. I really appreciate the mention of how it mimics anxiety because so many people feel dismissed by their doctors during the initial phase. We need to advocate for more holistic support systems that address the psychiatric toll alongside the hormonal one.
Olushola Adedoyin
April 24, 2026 AT 00:53The government is hiding the real cures! They want us on PTU because it makes us docile and easy to track with all those blood tests. This whole 'autoimmune' thing is just a cover for the strange signals they're pumping into the air to mess with our glands. Wake up people, the butterfly gland is being hijacked by the elites!
Valorie Darling
April 25, 2026 AT 01:44honestly just take the pills and stop whining about it lol like everyone has health issues and some of yall act like it's a tragedy that you gotta get blood work once a month. just do what the doctor says and move on with your life
Mike Beattie
April 26, 2026 AT 09:27The etiology of this condition is fundamentally a failure of immune tolerance, leading to the synthesis of TSI that acts as an agonist to the TSH receptor. If you're not optimizing your metabolic pathway through rigorous micronutrient supplementation, you're just treating the downstream effects. It's frankly amateur to ignore the synergistic impact of cortisol levels on the HPT axis while blindly trusting a standard dose of PTU.
Grace Grace
April 26, 2026 AT 09:39Oh my goodness, I can't even express how much this helps!! I went through the exact same thing with the shaking hands and it was the most terrifing expereince of my life. Please stay strong everyone and keep fighting for your helath, you are not alone in this battle!!
aman motamedi
April 26, 2026 AT 16:45I believe this information is presented with great clarity and provides a helpful service to those seeking a basic understanding of the condition.
Cynthia Didion
April 27, 2026 AT 05:11American medicine is the only gold standard for this. Period.
Aaron McGrath
April 28, 2026 AT 01:45CRUSH THOSE SYMPTOMS! You gotta be aggressive with your lifestyle changes while the ATDs do the heavy lifting! Optimize your VO2 max, lean into a high-protein regimen to combat the muscle wasting from hypermetabolism, and don't let the fatigue win! Get after it and force your body back into homeostasis through sheer will and clinical precision!
anne camba
April 29, 2026 AT 20:03The duality of the body's betrayal... is simply haunting...
Lucy Kuo
April 30, 2026 AT 06:40It is truly heart-rending to consider the immense suffering and psychological distress that accompanies such a diagnosis, yet there is a profound beauty in the way we can support one another through these tribulations. We must embrace a global perspective of care, ensuring that every individual, regardless of their origin, has access to these life-saving interventions. May we all find the strength to navigate these medical complexities with grace and an unwavering spirit of inclusivity and compassion for all afflicted souls!